Rehabilitation and Participation Science
Program in Occupational Therapy
by Stephanie Stemmler • September 16, 2021
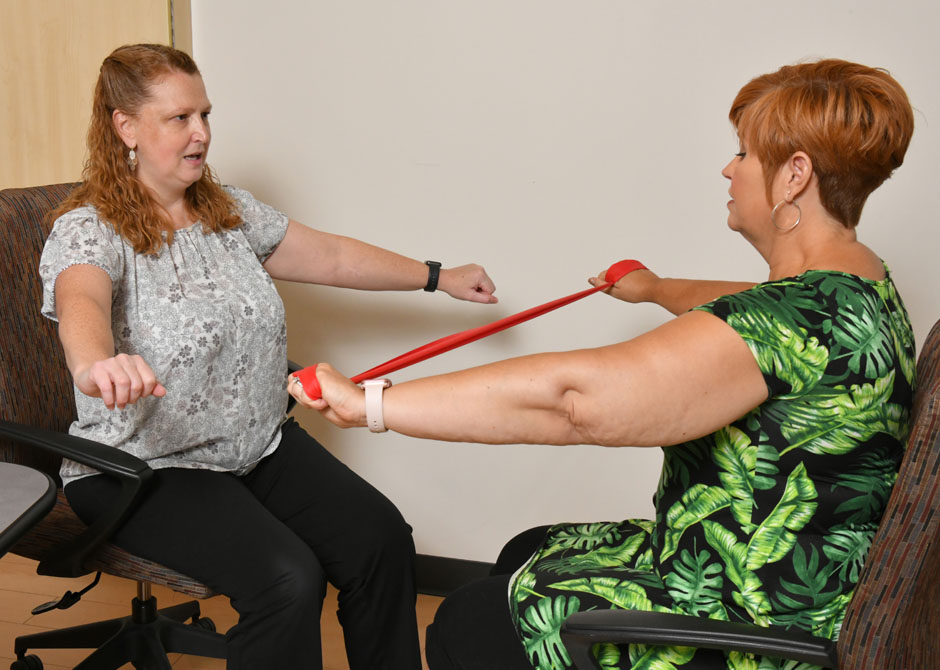
Karen Balk, MOT, OTR/L (left), reviews strengthening exercises with Amy Rustige (right) to improve posture to manage symptoms when sitting.
Within the past year, Karen Balk, MOT, OTR/L, has seen the number of patients referred to the Washington University Occupational Therapy Functional Neurological Disorders Program increase dramatically.
“When we started the program in mid-2019, we saw maybe five to 10 patients in that first year,” she says. “Now, after making presentations to neurologists and psychologists in the region and showing them how outpatient occupational therapy can help children and adults manage the symptoms associated with [functional neurological disorders], we see that many in just one week.”
Functional neurological disorders (FNDs) were once thought to be rare, affecting approximately 1 percent of the population. As awareness of the condition builds among health-care professionals (especially neurologists and psychologists), it is rapidly becoming one of the most common reasons for a neurological consult after headaches and migraines. In St. Louis, Washington University’s FND occupational therapy program is the only one of its kind in the region. Balk, who serves as lead therapist to this program, has found that such outpatient FND programs are virtually nonexistent. That needs to change, she believes, because patients clearly benefit from occupational therapy strategies to manage symptoms.
What is FND?
FNDs are characterized as a miscommunication, or dysfunction, in how the nervous system interacts between the brain and body. They are called “functional” because the symptoms manifest without a determined neurologic cause, such as a stroke or epileptic seizure. More than a decade ago, they were more commonly called “conversion disorders,” because the conventional thinking was that psychological stress or trauma converted to a physical symptom. In recent years, though, research has found that FNDs occur much like a software glitch, with certain parts of the brain signaling pathway malfunctioning and becoming stuck in a peculiar pattern, resulting in abnormal and dysfunctional movement, speech, breathing or gait problems.
“We tell our patients it’s a brain glitch,” explains Balk. “The brain somehow gets the sense that it needs a recurring symptom to create awareness so that the person realizes something needs to be addressed.”
Those “pokes” by the brain can be related to stress, illness, injury, accidents or abuse, or can result from physical triggers such as hunger, thirst, pain, body temperature, or noise or light problems. Most individuals can respond to such triggers without trouble, but in FND patients, the brain turns those trigger signals into a pattern of symptoms that keeps repeating. Symptoms can include limb weakness, tremors, spasms or gait problems, repetitive movements (dystonia), tics, speech problems, dissociative seizures or fainting episodes.
A 30-Year Puzzle
Amy Rustige was 19 years old when her pattern of abnormal symptoms started. “I was in college and had several headaches and a cold,” she recalls. “I woke up one morning and my whole arm kept making a waving motion that I couldn’t control.”
Over the next 30 years, Rustige would see multiple specialists trying to find answers. “I not only had the tremor and movement in my right arm, but also my left leg would freeze or make sudden movements, and then I developed problems with my diaphragm, which caused breathing complications,” she says.
At age 48, a chance referral to Washington University’s Movement Disorders Clinic led to a probable diagnosis of FND. As luck would have it, Balk, who had collaborated with the clinic to offer cognitive behavioral therapy for tics (CBIT), was launching her outpatient FND occupational therapy program. “I had seen a young client initially for a tic disorder and noticed that she had more than the usual symptoms for that, so I started to do research to figure out why,” Balk says.
Doctoral student Jackie Schechter, OTD ’20, was on her fieldwork rotation to help identify a handful of scholarly articles detailing treatment protocols for inpatient FND treatment. “In an inpatient setting, the ability to minimize distractions and keep patients focused in that structured environment was key to developing successful strategies,” says Balk. “What we wanted to do was develop an outpatient FND program because that was more aligned with everyday life.”
Retraining the Brain
Balk is focused on identification of FND triggers that cause symptoms and then micro-managing those so that the brain eventually “rewires” itself. It begins with reviewing individual symptoms and then having patients keep a detailed log of daily activities and sleep cycles as well as water and food intake for several weeks. Patients also note when FND symptoms occur. Balk then goes over the logs, noting common denominators that can be FND triggers.
“For example,” she says, “one client noted that her symptoms always began when it was cold in the morning. We told her to put on a warm bathrobe the minute she woke up, and that helped. Another client was able to effectively manage symptoms by being hyper-aware of heat and water intake.”
In Rustige’s case, learning to breathe in through her mouth and out through her nose successfully managed issues related to her diaphragm. Specific time-management skills reduced other symptoms. Balk even took measurements and duplicated Rustige’s home office where she works part-time as an illustrator, ultimately rearranging the workspace and changing the angle between Rustige’s chair and her desk to reduce fatigue.
Says Rustige, “For the first time in my life, she’s figured out the puzzle. That means I listen to my body more, take breaks and set limits on things so that I can go out with family members and spend time on more meaningful activities. Honestly, she gave me a lot of my life back.”
Balk has trained two additional therapists to work with FND patients. “I hope we set the standard for other programs nationwide to follow,” she says. “The need is great and, with the proper therapies, FND patients can remain within their homelife and work on improvements that enhance their day-to-day function and lives.”
We welcome inquiries from prospective students, potential collaborators, community partners, alumni and others who want to connect with us. Please complete the form below to begin the conversation.
Schedule an Info Session
We are excited that you are considering applying to the Program in Occupational Therapy at Washington University. Please join us for a Zoom Information Session for either our entry-level MSOT or OTD degrees or our online Post-Professional OTD. Current faculty members will discuss the degree program and answer any question you may have. We are offering these sessions on the following days and times. The content is the same for each one, so you only need to sign up for one.
Upcoming ENTRY-LEVEL Degree ZOOM Info sessions:
Schedule an Entry-Level Info Session
Upcoming PP-OTD Degree ZOOM Info session: