Rehabilitation and Participation Science
Program in Occupational Therapy
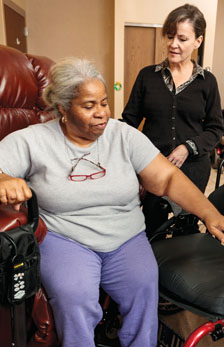 Susy Stark, PhD, OTR/L, FAOTA, says her mission is “to develop evidence-based interventions designed to improve aging in place safely and promote the implementation of those interventions by occupational therapists (OTs).”
Susy Stark, PhD, OTR/L, FAOTA, says her mission is “to develop evidence-based interventions designed to improve aging in place safely and promote the implementation of those interventions by occupational therapists (OTs).”
Translation — she wants to make the world a better place. Stark, an associate professor of occupational therapy, neurology and of social work, is director of the Participation, Environment and Performance Laboratory in the Program in Occupational Therapy at Washington University School of Medicine. An internationally recognized clinician and translational scientist, Stark has spent almost her entire career trying to harness what she calls a “superpower” in helping older adults live more independently in their homes and remain active in their communities.
“It’s so obvious once you start thinking this way,” she says. “It’s the environment. As I worked with patients and conducted research in the community, I could clearly see that if we could fix or modify aspects of a person’s environment, they could do what they wanted to do and remain as independent and engaged as possible. For them, a modified environment was their superpower for them to keep living how they wanted.”
Early in her career, Stark said, it was an unusual concept to focus on the environment and its impact on functional limitations and disabilities. “At first, we couldn’t imagine changing the environment to support performance,” she recalls. “But then came the Americans with Disabilities Act, the civil rights law passed in 1990 that prohibited discrimination against people with disabilities. While that was exciting, buildings still were being constructed with steps, which impacted accessibility. It just didn’t make sense. I kept asking myself, ‘Why wasn’t everyone focused on the environment?’”
Stark said that question ultimately pushed her to pursue a doctorate in environment and behavior science from the University of Missouri. “My dissertation was on the environmental barriers and support in homes of people with disabilities, which made me realize that through informed practice, we could track outcomes and change practices worldwide, thereby enhancing the quality of life for many, many people.”
Stark initially earned her master’s degree from the Program in Occupational Therapy in 1989. She served as an OT at Washington University (WashU), working with a wide variety of patients, including homeless individuals, mentally ill women, older adults after hip fracture, and kids with behavioral disorders. After leaving to obtain her doctorate, Stark returned to WashU to work with David Gray, PhD, a psychologist known internationally for his efforts to improve the lives of people with disabilities. Stark worked with Gray, who died in 2015, to develop a series of survey instruments designed to assess physical environmental features and identify barriers that impact the participation of individuals with mobility impairments, low vision or hearing loss.
“It was eye-opening,” says Stark, who subsequently focused her own research on older adults, wondering if home modifications could positively influence functional ability and independence for seniors at risk for falling. The research was significant because in the U.S. alone, one in three older adults fall every year, with half of those falls taking place in the home.
Her research was among the first in the U.S. to empirically show that, yes, home modifications can significantly improve function, and subsequently, independence, among older adults with chronic conditions. Pushing those results directly into the community, Stark collaborated with the Jewish Federation of St. Louis to establish the St. Louis Naturally Occurring Retirement Community (NORC) in 2004. The senior living community enables adults to more easily age in place and engage in community activities with the use of home modifications. NORC now has been a model community in St. Louis for more than 13 years.
We welcome inquiries from prospective students, potential collaborators, community partners, alumni and others who want to connect with us. Please complete the form below to begin the conversation.
Schedule an Info Session
We are excited that you are considering applying to the Program in Occupational Therapy at Washington University. Please join us for a Zoom Information Session for either our entry-level MSOT or OTD degrees or our online Post-Professional OTD. Current faculty members will discuss the degree program and answer any question you may have. We are offering these sessions on the following days and times. The content is the same for each one, so you only need to sign up for one.
Upcoming ENTRY-LEVEL Degree ZOOM Info sessions:
Schedule an Entry-Level Info Session
Upcoming PP-OTD Degree ZOOM Info session: